 
Here are other specifics that the newly proposed rule would do if it became effective: The rule also addresses congressional directives that were enacted in recent legislative efforts. If finalized, it would also clarify and strengthen existing regulations called for in the Mental Health Parity and Addiction Equity Act (MHPAEA), a law passed in 2008 that sought to prevent health plans from treating behavioral health benefits differently than physical health benefits. “Health educators, including parents themselves, may need to develop plans to educate adolescents earlier about mental health concerns given the increasing rates of acute care events,” he said.The proposed rules would incorporate provisions from several laws passed by Congress as well as the experience of several federal agencies since the last major overhaul of mental health parity rules in 2014. With so many young people affected by mental health challenges, many of which begin in high school, Brennan suggests that parents, mental health professionals, and community members need to be aware of changing environmental factors that may exacerbate mental health challenges for teens. The pandemic has only exacerbated this towering demand.” That’s well over a 100 million ‘silent sufferers’-people who need or would greatly benefit from therapy but don’t get help due to stigmatization, access, costs, or other factors. “There is compelling data indicating that over 150 million Americans suffer annually from a range of mental and behavioral health issues, yet only one in four seeks out treatment. “Well before the pandemic took hold, the nation was already in the throes of a major mental health crisis,” said Dale Cook, cofounder and CEO of Learn to Live, a digital mental health platform. Insufficient numbers of mental health providers is a broader problem than in Medicaid alone, particularly as demand for mental health care has ballooned during the pandemic. More emergency room visits and fewer office visits may imply that there are not enough pediatric mental health providers who accept Medicaid to serve all kids who need mental health care. The data on kids with Medicaid suggests a troubling dynamic. Mental health office visits and outpatient care increased by nearly one-third for children with private insurance but declined by 2% among children on Medicaid. But rates of outpatient service utilization were substantially different by type of health insurance. Overall, use of outpatient mental health services increased by just 5% between 20, including sharp declines in 2020 with the onset of the pandemic. “This points to not having adequate numbers of mental health professionals accepting Medicaid patients, as well as the general failure to integrate behavioral health into the primary care and school-based supports provided to these children,” he said. These findings surprised the Clarify Health team, according to Brennan. Emergency room visits increased by 20% among children on Medicaid but actually declined 10% among privately insured kids.  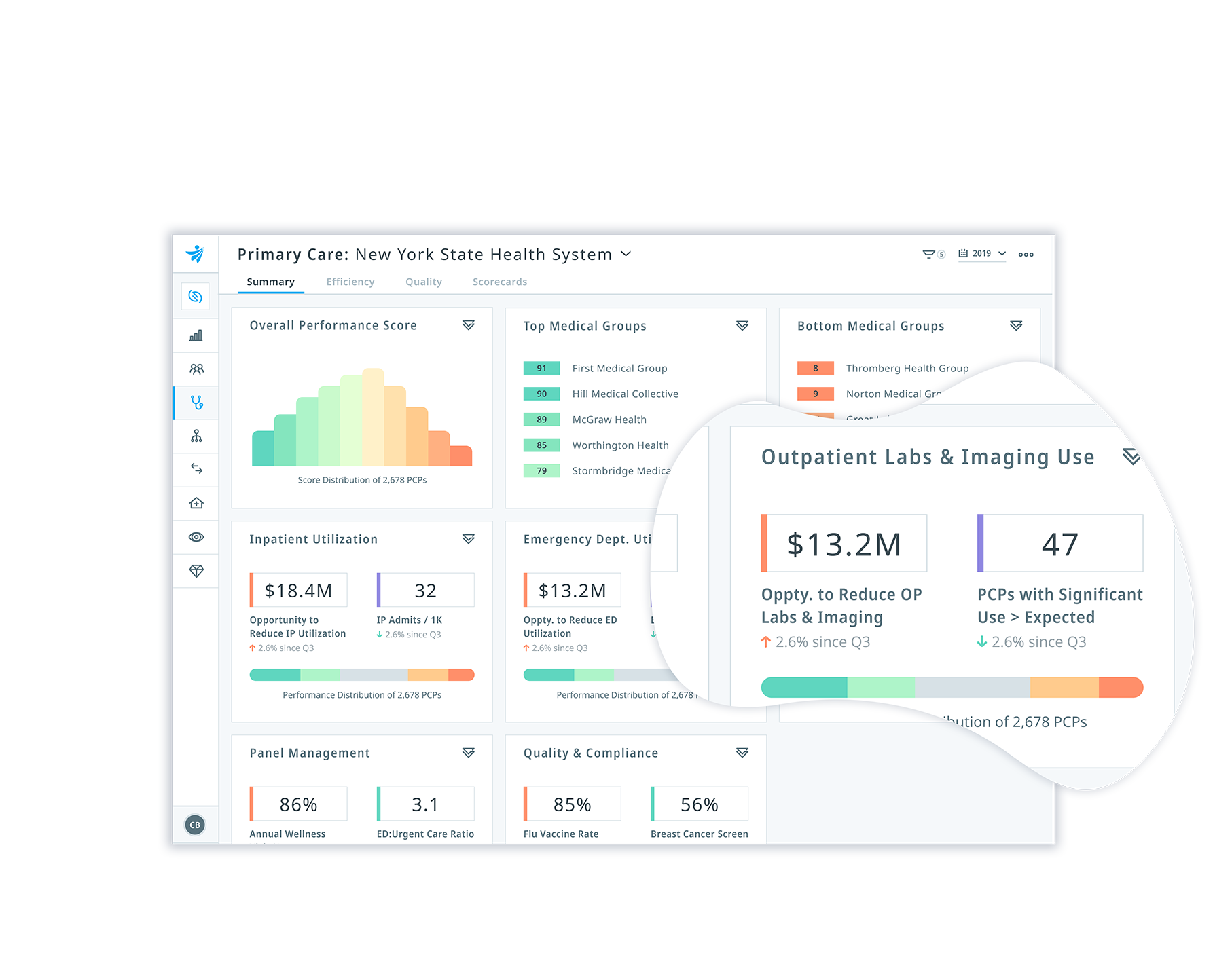
On the other hand, children on Medicaid used the emergency room twice as much as kids with private insurance. Hospitalizations doubled among kids with commercial health insurance but increased 40% among kids on Medicaid, the publicly funded health insurance program for lower-income people. The analysis found differences in mental health service usage by health insurance coverage. 
“The growth in acute mental health events we document should be a serious concern for parents, and thus should be of concern to their employers, government officials, and other community leaders,” Brennan said. Emergency room usage jumped 41% among 12-to-15 year old girls and 35% among boys. Adolescents between 12 and 15 years of age were more likely to have visited an emergency room during this time compared to younger and older kids. But the current lack of beds creates serious unmet needs across geographies and sociodemographic groups.Įmergency room visits due to mental health conditions increased by 20% between 20, also spiking during the pandemic after an initial decline early on in the five-year period included in the data. The West North Central region had a 27% increase in mental health hospitalizations, the lowest increase of any region.Īccording to Brennan, many health systems around the country are seeking to increase the availability of pediatric hospital beds. While hospitalizations went up in all regions of the United States, they increased the most in the mid-Atlantic and New England, which had 137% and 100% increases, respectively. The analysis also found substantial regional differences in rates of increase in hospitalizations for pediatric mental health conditions. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
